Tuesday, December 9, 2008
Contrast Media Administration Guidelines by the ACR (American College of Radiology) Version 6 - 2008
Contrast Media Administration Guidelines by the ACR (American College of Radiology) Version 6 - 2008
Sunday, December 7, 2008
Friday, December 5, 2008
Fwd: Three MRI Images with gadolinium
---------- Forwarded message ----------
From: himadri das <drhsdas@gmail.com>
Date: Fri, Dec 5, 2008 at 7:21 PM
Subject: Re: Three MRI Images with gadolinium
To: Lenny & Lynne Camera <ljjc@verizon.net>
Hi,
As regards to your mail , I dont know whether I shuold be answering this but anyways- every things to be correlated with history, signs , symptoms & actual temporal cascade of events leading the patient to to CT or MR suites.My off the record & personal observations would be:
E5: Yes could be cortical venous thrombosis and/or focal cerebritis. Infection from the left frontal sinus will however have to pierce the bones & the dura so few CT sections might help.
28: mild bilateral maxillary sinus disease. however the airspaces of the nasal cavities are reduced due to DNS & hypertrophied turbinates leading to nasal blockage ( if any ) compounding the sinus disease. The sinus ostia ( OMU) shuld be observed to see whether patency is maintained.
43: I feel its bilateral maxillary mucosal thickening with polypoidal component anteriorly on the right side.
Regards & best wishes,
Dr H.S.Das
From: himadri das <drhsdas@gmail.com>
Date: Fri, Dec 5, 2008 at 7:21 PM
Subject: Re: Three MRI Images with gadolinium
To: Lenny & Lynne Camera <ljjc@verizon.net>
Hi,
As regards to your mail , I dont know whether I shuold be answering this but anyways- every things to be correlated with history, signs , symptoms & actual temporal cascade of events leading the patient to to CT or MR suites.My off the record & personal observations would be:
E5: Yes could be cortical venous thrombosis and/or focal cerebritis. Infection from the left frontal sinus will however have to pierce the bones & the dura so few CT sections might help.
28: mild bilateral maxillary sinus disease. however the airspaces of the nasal cavities are reduced due to DNS & hypertrophied turbinates leading to nasal blockage ( if any ) compounding the sinus disease. The sinus ostia ( OMU) shuld be observed to see whether patency is maintained.
43: I feel its bilateral maxillary mucosal thickening with polypoidal component anteriorly on the right side.
Regards & best wishes,
Dr H.S.Das
On Thu, Dec 4, 2008 at 8:10 PM, Lenny & Lynne Camera <ljjc@verizon.net> wrote:
Can you explain what you see in these three images. The first image 14B68928, December 24, 2007.....is this case of sinusitis/maxillary disease considered severe? On Second image 051FEFE5 Question.......could the cloudy white spot in the upper left frontal be an abscess from the sinuses? On Image 041A7943 and 14B68929 could it be not totally sinusitis, could some of it be pooling from a small CSF leak due to trauma?Thank you
Friday, November 21, 2008
NEURO – IMAGING IN PSYCHIATRY
NEURO – IMAGING IN PSYCHIATRY
Dr Himadri Sikhor Das
In psychiatry Neuroimaging is primarily used to aid in differential diagnosis. The clinical value of neuroimaging is used to demonstrate underlying organic brain pathology as a possible cause of disturbed mental status. Pathognomonic image profiles indicative of specific psychiatric disorders have not yet been fully identified; thus for the time being neuroimaging studies are finding only limited utility in identification of specific primary psychiatric diseases. In the future, however neuroimaging techniques may be used to make or confirm psychiatric diagnoses and neuroimaging profiles may be incorporated into the diagnostic criteria of certain psychiatric disorders. However in the future, imaging data may be valualable for predicting natural courses of illness as well as monitoring response to treatment.
MRI IMAGING IN PSYCHIATRIC ILLNESSES: -
Although specific clinical decisions must be mode on a case-to-case basis, tentative guidelines regarding the indications for structural neuroimaging in psychiatry have been suggested. These should be considered for patients who meet any of the four following criteria: -
1. Acute mental status change (including those of affect, behaviors or personality), plus any of:
- Age > 50 years
- Abnormal neurological examination.
- History of significant head trauma (i.e. Head trauma resulting in loss of consciousness or neurological sequelae)
2. New onset psychosis
3. New onset delirium or dementia of unknown etiology.
4. Prior to an initial course of ECT.
In addition to the above which focus on acute presentation; neuroimaging should also be considered when a patient’s distorted metal status proves refractory. Following these criteria a very low proportions of brain lesion associated with treatable general medical conditions could be missed. Move specifically, older age groups, psychiatric inpatients and patients with co-morbid medical illness likely will present the highest rate of positive findings. Finally an even higher percentage of patients may benefit from negative findings in a more subtle fashion i.e., as a consequence of the reassurance attained from having gross structural pathology ruled out and the primary psychiatric diagnoses solidified.
ROLE OF MRI IN CLINICAL NEUROSCIENCE: -
MRI is seen to play an important role in clinical neuroscience research in psychiatry. In general studies are done with two aims: -
- First images from large cohorts of patients and comparison subjects are reserved in order to identity pathological change that occurs in ill individuals.
- Second general research approach in to ask focused questions about the volume or shape of specific brain tissue types or structure to provide evidence regarding the involvement of these structures in the pathophysiology of specific conditions.
RECENT IMAGING MODALITIES: Recent advances in NMR and nuclear medicine techniques are finding more and more importance in pursuing active research work in Psychiatric diseases as well providing new insights into the human brain. With the advent of functional imaging, processes like memory, emotion, thought etc are being researched by scientists all over the world.
I. NUCLEAR MEDICINE (PET/SPECT):
Nuclear medicine procedures used for diagnosis and research of psychiatric conditions generally utilize PET and SPECT scans. These methods show blood flow by imaging trace amounts of radioisotopes. PET however can measure metabolism revealing how well the body is functioning. Use of radioactive tracers is well suited to studies of epilepsy, schizophrenia, Parkinson’s disease and stroke. Both PET and SPECT depict the distribution of blood into tissues, but PET does so with greater accuracy.
PET scanners watch the way the tissue cells (eg. brain cells) consume substances such as sugar (glucose). The substance is tagged with a radioisotope and brewed in a small, low energy cyclotron. The isotope has a small half-life meaning it loses half of its radioactivity only within minutes or hours of being created. Injected into the body the radioactive solution emits positrons wherever it flows. The positrons collide with electrons and the two annihilate each other releasing a burst of energy in the form of two gamma rays. These rays shoot in opposite directions and strike crystals in a ring of detectors around the patient’s head causing the crystals to light up. A computer records the location of each flash and plots the source of radiation, translating the data into an image. By tracing the radioactive substance a doctor can pinpoint areas of abnormal brain activity or determine the health of cells. Unlike PET, which specially requires a cyclotron on site, SPECT uses commercially available radioisotopes greatly reducing the cost of operation.
II. FUNCTIONAL MAGNETIC RESONANCE IMAGING (FMRI) IN PSYCHIATRY.
First, the most commonly used fMRI technique called BOLD-fMRI (Blood-Oxygen-Level-dependent fMRI) potentially offers imaging with a temporal resolution on the order of 100 milliseconds and a spatial resolution of 1-2 millimeters, which is much greater than that of PET and SPECT scanning. This means that transient cognitive events can potentially be imaged and small structures like the amygdala can be more readily resolved. Most fMRI techniques are noninvasive and do not involve the injection of radioactive materials so that a person can be imaged repeatedly. This allows imaging of a patient repeatedly through different disease states (i.e. imaging a bipolar patient through manic, depressive, and euthymic states) or developmental changes (ie. Learning cognitive stages of development, stages of grief recovery). Third, with fMRI, one can easily make statistical statements in comparing different mental states within an individual in a single session. Thus, fMRI may be of important use in understanding how a given individual’s brain functions and perhaps, in the future, making psychiatric diagnoses and treatment recommendations. It is in fact already starting to being used in presurgical planning to map vital areas like languages, motor function, and memory.
The four main applications of MRI yielding functional information in psychiatry can be categorized as: -
1. BOLD-fMRI that measures regional differences in oxygenated blood.
2. Perfusion fMRI, which measures regional cerebral blood flow.
3. Diffusion-weighted fMRI which measures random movement of water molecules and
4. MRI spectroscopy, which can measure certain cerebral metabolites noninvasively.
1. BOLD-fMRI (BLOOD-OXYGEN-LEVEL-DEPENDENT FMRI):
BOLD-fMRI is currently the most common fMRI technique. With this technique, it is assumed that an area is relatively more active when it has more oxygenated blood compared to another point in time. This is based on the principle that when a brain region is being used, arterial oxygenated blood will redistribute and increase to this area. BOLD fMRI is a relative technique in that it must compare images taken during one mental state to another to create a meaningful picture. As images are acquired very rapidly (ie. a set of 15 coronal brain slices every 3 seconds is commonly) one can acquire enough images to measure the relative differences between two states to perform a statistical analysis within a single individual. Ideally, these states would differ in only one aspect so that everything is controlled for except the behavior in question.
BOLD fMRI paradigms generally have several periods of rest alternating with several periods of activation. Images are then compared over the entire activation to the rest periods. BOLD fMRI is best used for studying processes that can be rapidly turned on and off like language, vision, movement, hearing and memory.
BOLD fMRI is very sensitive to movement so that tasks are limited to those without head movement, including speaking. BOLD fMRI is also limited in that artifacts are often present in brain regions that are close to air (ie. sinuses). Thus there are some problems in observing important emotional regions at the base of the brain like the orbitofrontal and medial temporal cortices. Another problem is that sometimes observed areas of activation may be located more in areas near large draining veins rather than directly at a capillary bed near the site of neuronal activation.
Currently, there are no indications for BOLD fMRI in clinical psychiatry, although this technique holds considerable promise for unraveling the neuroanatomic basis of psychiatric disease. It may be of potential help in sorting out diagnostic heterogeneity and treatment planning in the future. Neurologists and neurosurgeons are beginning to use this technique clinically to noninvasively map language, motor and memory function in patients undergoing neurosurgery.
2. PERFUSION fMRI:
Two fMRI methods have been developed for measuring cerebral blood flow. The first method, called intravenous bolus tracking, relies on the intravenous (iv) injection of a magnetic compound such as a gadolinium-containing contrast agent and measuring its T2 weighted signal as it perfuses through the brain over a short time period of time.
Areas perfused with the magnetic compound show less signal intensity as the compound creates a magnetic inhomogeneity that decreases the T2 signal. The magnetic compound may be injected once during the control and once during the activation task and relative differences in blood flow between the two states may be determined to develop a perfusion image. Alternatively one can measure changes in blood few over time over time after a single injection to generate a perfusion map.
This technique also only generates a map of relative cerebral blood flow, not absolute flow as in the text technique. Arterial spin labeling is a T1 weighted noninvasive technique where intrinsic hydrogen atoms in arterial water outside of the slice of interest are magnetically tagged (“flipped”) as they course through the blood and are then imaged as they enter the slice of interest.
Arterial spin labelling is noninvasive, does not involve an IV bolus injection, and can, thus, be repeatedly performed in individual subjects. Also, absolute regional blood flow can be measured which cannot be easily measured with SPECT or BOLD fMRI and requires an arterial line with PET. As absolute information is obtained, cerebral blood flow can be serially measured over separate imaging sessions such as measuring blood flow in bipolar subjects as they course through different disease states. Absolute blood flow information may be important in imaging such processes as anxiety, which may be hard to turn on and off. For instance, in social phobics, a relaxation task may be imaged on one day and anticipating making a speech may be imaged on the next day. Comparing these separate tasks in different imaging sessions would not be possible with BOLD fMRI. Arterial spin labelling has some limitations in that it takes several minutes to acquire information on a single slice of interest. Therefore, one must have a specific brain region that one is interested in examining. Also, as it currently takes several minutes to acquire a single slice, it would be tedious obtaining enough images on this slice within a single session to make a statistical statement on a given subject.
3. DIFFUSION-WEIGHTED IMAGING (DWI)
Diffusion-weighted imaging is very sensitive to the random movement of 1 H in water molecules (Brownian movement). The amount of water diffusion for a given pixel can be calculated and is called the apparent diffusion coefficient (ADC). Areas with low ADC value (ie. low diffusion) appear more intense. ADC values are direction sensitive. While it is currently unclear now diffusion-weighted imaging will be useful in studying psychiatric disorders, it hold great promise for changing the clinical management of acute ischaemic stroke by potentially refining the criteria for patients most likely to benefit from thrombolytic therapy.
4. MRI SPECTROSCOPY (MRS):
MRI spectroscopy (MRS) offers the capability of using MRI to noninvasively study tissue biochemistry. In the conventional and functional MRI techniques listed. The hydrogen atom in water is the main one that is flipped (resonated). In MRS, either 1H atoms in other molecules or other atoms such as 31P, 23Na, K, 19F or Li are flipped. Within a given brain region called a voxel, information on these molecules is usually presented as a spectrograph with precession frequency on the x-axis revealing the identity of a compound and intensity on the y-axis, which helps quantify the amount of a substance. The quantity of a substance is related is related to the area under its spectrographic peak; the larger the area, the more of a substance that is present.
The two most widely used MRS techniques involve either viewing 1H atoms in molecules other than water or 31P-containing molecules. In 1H MRS, the water signal must first be suppressed as it is much greater than the signal from other 1H-containing compounds and has overlapping spectroscopic peaks with compounds.
Compounds that can be resolved with 1H-MRS include:
a) N-acetylaspartate (NAA) which is though to be a neuronal marker that decreases in processes where neurons die;
b) Lactate which is a product of anaerobic metabolism and may indicate hypoxia;
c) Excitatory neurotransmitters glutamate and aspartate;
d) The inhibitory neurotransmitter gamma-amino butyric acid (GABA);
e) Cytosolic choline which includes primarily mobile molecules involved in phospholipid membrane metabolism but also small amounts of the neurotransmitter acetylcholine and its precursor choline;
1. Myolinositol which is important in phospholipoid metabolism and intracellular second messenger systems; and
2. Creatine molecules such as creatine and phosphocreatine, which usually have relatively constant concentrations throughout the brain and are often used as relative reference molecules (ie. one may see NAA concentration reported as the ratio NAA/creatine in the literature).
Phosphorus (31P) MRS allows the quantification of ATP metabolism, intracellular pH, and phospholipid metabolism. Mobile phospholipid, including phosphomonoesters (PME - putative cell membrane building blocks) and phosphodiesters (PDE – putative cell membrane breakdown products) can also be measured, supplying information on phospholipid membrane metabolism.
MRS can be used to identify regional biochemical abnormalities. For example, P-MRS studies of euthymic bipolar patients have revealed decreased frontal lobe PMEs (cell membrane building blocks) compared with healthy controls. However, when bipolar patients become either manic or depressed, their PMEs increase.
These findings appear to be unrelated to medication treatment. The finding of decreased frontal PMEs in euthymic bipolars has also been demonstrated in schizophrenia and speculatively accounts for the finding of decreased frontal lobe metabolism in both of these disorders. The schizophrenia finding also appears to be medication-independent.
MRS may also be of future help in the differential diagnosis of certain psychiatric diseases such as dementia. In normal aging, there is a decrease in PMEs and increase in PDEs. In early Alzheimer’s Dementia compared with healthy controls. Some believe that a decrease in NAA coupled with an increased myoinositol lever helps in differentiating probable Alzheimer’s Dementia from healthy age-matched controls as well as other dementias (usually decreased NAA but normal myoinositol levels).
With MRS, changes in metabolic activity can be measured over time within an individual scanning session. MRS can also be used to measure changes in metabolic activity between sessions, such as before and after medication treatment. For example, Satlin et al. (1997) used 1H MRS to measure midparietal lobe cytosolic choline levels in 12 Alzheimer’s subjects before and after treatment with Xanomeline, an M1 selective cholinergic agonist, or placebo. Additionally, MRS can be used to measure drug levels of certain psychotropic drugs. The magnetic elements Li and F do not naturally occur in the human body but they are fund in psychotropic drugs; lithum for Li and fluoxetine and stelazine for F. For example, studies have consistently found that the brain concentrations of lithium are about 0.5 that of serum Li levels and correlate with treatment response.
For psychiatry, MRS is a research to be used in the characterization of tumor, stroke and epileptogenic tissue and in presurgical planning.
LIMITATIONS:
MRS is restricted to studying mobile magnetic compounds. As neurochemical receptors are noted usually mobile, they cannot be measured with MRS. Thus, receptor-ligand studies are still the domain of SPECT and PET. Another problem with MRS is that due to the low concentrations of many of the imaged substances, larger areas than with water are needed to obtain detectable signals. Larger volume units imaged over longer periods are thus used with this technique, limiting both temporal and spatial resolution compared with conventional MRI and BOLD-fMRI. However, stronger magnetic fields which can spread out precession frequencies over a wider range may improve this resolution.
A brief view of recent findings are outlined.
PSYCHOTIC DISORDERS:
Research studies have identified a large number of pathologies in at last some subjects of schizophrenia for eg, the main regions sharing consistent abnormalities in schizophrenia have been frontal & temporal lobe structures. Volume decreases have been found in 62% of 37 studies of the whole temporal lobe, in 81% of 16 studies of the superior temporal gyrus and in 77% of 30 studies of the medial temporal lobe. Temporal lobe volume reduction may be uni or bilateral with deficits observed more commonly in left temporal lobe. Frontal lobe volume reductions have been reported in 55% of all published studies. Regional volume reductions have been reported in thalamus and corpus callosum. Interestingly, basal ganglia volumes may increase during treatment with typical, but not atypical neuroleptic agents. Recently studies in children have also shown findings consistent with the adult findings.
MOOD DISORDERS:
Major Depression
The spectrum of affective illness is very broad, ranging from single episodes of depressed mood, which are self-limited to life-long, treatment-refractory despondency with recurrent suicidality. Proposed that both primary and secondary mood disorders may involve abnormalities in specific frontosubcortical circuits that regulate mood. Depression is observed frequently in persons with degenerative diseases of the basal ganglia, such as Huntington’s disease, Parkinson’s disease, Wilson’s disease.
In older adults, frontal lobe atrophy and an increasing burden of T2 weighted, high signal intensity lesions have been correlated with late-life depression. Evidence suggests that depression may be seen following focal damage to critical brain regions as well as in response to diffuse brain injury. As the amygdala plays a key role in the brain’s integration of emotional meaning with perception and experience, volumetric studies of this brain structure currently are being reported. Sheline et al. have observed decreased amygdalar core nuclei volumes in depressed subjects increased amygdalar volumes in depressed patients. Mervaala et al. have noted significant amygdalar asymmetry (right smaller than left) in severely depressed subjects.
Strokes and tumors located in left sided frontal regions have been associated with new onset depression and less commonly; right-sided lesions may lead to manic symptoms. Subcortical lesions, especially of the caudate and thalamus, also can lead to mood dysregulation, with right sided lesions again being more commonly associated with mania. 30 MR studies with most consistent finding observed in 10 of 12 studies is a three-fold increase in the presence of WMH. The etiology of these WMH in bipolar patients is not clear, rates of alcohol and substance abuse, smoking cardiovascular risk factors contribute. As in schizophrenia some patients with bipolar disorder have increased lateral and third ventricular volume. Brain regions with volume deficits in bipolar include the cerebellum, especially in patients who are older or how have had multiple episodes of mania toxic effects of alcohol abuse lithium treatment.
Reduced volume and altered activity of subgenual prefrontal cortex in familial bipolar disorder has been reported. Subgenual cingulate cortex volume more recently increased amygdalar volumes have been seen in persons with bipolar disorder. Limited available data suggest that panic attacks may arise, in a minority of cases, as a consequence of ictal activity and that brain MR may identify a reasonably high yield of septo-hippocampal abnormalities in the subpopulation of panic patients who also have electroencephalogram abnormalities. Emission tomography studies generally have observed increased orbitofrontal and cingulate blood flow and glucose utilization, with decreased caudate perfusion. Hippocampal volume reductions on the order of 5% to 12% have been reported, which are of a lesser magnitude than those observed in AD or temporal-lobe epilepsy.
Neuroimaging studies of Dementing illness constitute a very active area of ongoing research. A great deal of attention has been paid to the hippocampus, as progressive atrophy has been reported to correlate with memory loss in a number of studies of both healthy adults and individuals with dementing illnesses. Recently have suggested that other regions of interest (e.g. entorhinal cortex, anterior cingulate and the banks of the superior temporal sulcus) may show larger rates of change in structural volume, over the for the hippocampal formation. Assessment of the medial occipitemporal, inferior and middle temporal gyri in demented elderly also has been suggested as a means to predict progression to AD. Alternatively, measurement of global cerebral volume also has been proposed as a means to assess disease progression. In healthy older adults, ventricular volume has been shown to increase by approximately 1.5 cm / year, suggesting that brain tissue loss is relatively slow in the absence of degenerative disorders. Frontotemporal dementia (FTD) may be distinguished from AD on the basis of anterior hippocampal atrophy (AD).
Decreases in the area of the body and posterior subregions of the corpus callosum have been reported in autistic individuals. Anorexia nervosa has been strongly associated with cerebral ventricular enlargement as well as gray and white matter deficits. Refeeding is associated with some improvement in ventricular and white matter volumes but gray matter volume deficits tend to persist, as do some neurocognitive impairments. Anorexia and bulimia may be associated with hyponatremia, which can lead to the development of central pontine myelinolysis.
Substance Use Disorders.
Alcohol-induced ventricular and sulcal enlargement have been observed by many. Regional atrophy of the corpus callosum and the hippocampus also have been reported. The cerebellum appears to be particularly sensitive to alcohol-induced damage. In addition to atrophic changes, diffuse white matter hyperintensities, suggestive of demyelination have been observed in T2 weighted examination of asymptomatic alcoholics. Signal intensity changes within the globus pallidus also have been observed in persons with cirrhosis, which may improve following liver transplantation.
Wernicke korsakoff syndrome results from nutritional deficiencies and may be precipitated by glucose administration to thiamine deficient alcoholics. The neuroanatomic change most closely associated with Wernicke Korsakoff syndrome in mamillary body atrophy although regional changes in the thalamus, orbitofrontal cortex and mesial temporal lobe also have been reported. Central pontine myelinolysis often is detected in alcoholics and presumably arises from rapid correction of electrolyte imbalance in severe hyponatremia. Extrapontine lesions also may be observed in CPM patient, affecting the cerebellar peduncles, basal ganglia and the thalamus. Marchiafava Bignami disease is a rare hemispheric disconnection syndrome typically associated with chronic alcoholism. MBD often is associated with hypointense T1 weighted or hyperintense T2 weighted lesions of the corpus callosum, suggestive of demyelination. Alcohol discontinuation and nutritional supplementation may contribute to recovery from MBD.
Stimulant Dependence.
Cocaine dependence recently has been associated with an increased incidence of WMH on T2 weighted imaging studies an incidence rate for asymptomatic stroke of approximately 3% in abstinent former cocaine users. Abuse of amphetamine and methampetamine also have been associated with cerebral ischaemia.
Other Drugs
Lipophilic adulterants present in preparations of vaporized heroin may produce signs of a toxic leukoencephalopathy. Chronic use of combined heroin and cocaine has been associated with increased pituitary volume as well as reduced prefrontal and temporal cortex volume. Solvent abuse has been linked to loss of gray white matter tissue differentiation, increased perivascular white-matter signal hyperintensities and cerebral atrophy.
CONCLUSIONS:
While there are currently no clinical indications for ordering any of these fMRI techniques, they hold considerable promise for unraveling the neurocircuitry and metabolic pathways of psychiatric disorders in the immediate future and in further helping in psychiatric diagnosis and treatment planning.
REFERENCES:
1. Magnetic resonance imaging of Brain and spine, Third Edition, Volume – I, 2002, chapter 22, Page no = 1189-1205
2. Posse S, Muller-Gartner HW, Dager SR. Functional Magnetic Resonance Studies of Brain Activation. Seminars in Clinical neuropsychiatry 1996; 1:76-88.
3. Bonder JR, Swanson SJ, Hammeke TA Morris GL, Myeller WM, Fischer M, et al. Determination of language dominance using functional MRI: A comparison with the Wada test. Neurol 1996; 46:978-984.
4. Moseley ME, Decrespigny A, Spielman DM. Magnetic Resonance Imaging of Human Brain Function. Surgical neurology 1996; 45:385-391.
5. David A, Blamire A, Breiter H. Functional Magnetic Resonance Imaging: A new technique with implications for psychology and psychiatry. Brit J Psychiatry 1994: 164:2-7.
6. Menon RS, Ogawa S, Hu X, Strupp JP, Anderson P, Ugurbil K. BOLD based functional MRI at 4 Tesla includes a capillary bed contribution: echo-planar imaging correlates with previous optical imaging using intrinsic signals. Magn Res Med 1995; 33: 453-459
7. Belliveau JW, Kennedy DN, McKinstry RC, Buchbinder BR, weisskoff RM, Cohen MS, et al. Functional mapping of the visual cortex by MRI. Science 1991; 254: 716-719.
8. Harris GJ Lewis RF, Satlin A, English CD, Scott TM et al. Dynamic susceptibility contrast MRI of regional cerebral blood volume in Alzheimer’s disease. Am J psychiatry 1996; 153: 721-724
9. Fisher M, Prichard JW, Warach S. New magnetic resonance technique for acute ischaemic stroke, JAMA 1995; 274:908-911
10. Zivan JA. Diffusion-weighted MRI for diagnosis and treatment of ischaemic stroke. Ann neurol 1997;567-568
11. Moore CM, Renshaw PF. Magnetic Resonance Spectroscopy Studies of Affective Disorders. In: Krishnan KRR, Doraiswarmy PM, editors. Brain Imaging in Clinical Psychiatry. New York : marcel-Dekker, 1997:185-213
12. Frangou S, Williams SC. Magnetic resonance spectroscopy in psychiatry: Basic principles and applications. British Medical Bulletin 1996 ; 52:474-485
13. Pettigrew JW, withers G, panchalingam K, post JF. 31P nuclear magnetic resonance (NMR) spectroscopy of brain in aging and Alzheimer’s disease. J Neural Transm Suppl 1987; 24:261-268
14. Functional magnetic resonance imaging (fMRI) for the pshychiatrist Lorberbaum JP, Bohning DE, Shastri A, Nahas Z et al.
15. Dager SR, Strauss WL, Marro KI Richards TL, Metzger GD et al. Proton Magnetic resonance spectroscopy investigation of hyperventilation in subjects with panic disorder and Comparison subjects. Am J psychiatry 1995; 152:666-672
Dr Himadri Sikhor Das
In psychiatry Neuroimaging is primarily used to aid in differential diagnosis. The clinical value of neuroimaging is used to demonstrate underlying organic brain pathology as a possible cause of disturbed mental status. Pathognomonic image profiles indicative of specific psychiatric disorders have not yet been fully identified; thus for the time being neuroimaging studies are finding only limited utility in identification of specific primary psychiatric diseases. In the future, however neuroimaging techniques may be used to make or confirm psychiatric diagnoses and neuroimaging profiles may be incorporated into the diagnostic criteria of certain psychiatric disorders. However in the future, imaging data may be valualable for predicting natural courses of illness as well as monitoring response to treatment.
MRI IMAGING IN PSYCHIATRIC ILLNESSES: -
Although specific clinical decisions must be mode on a case-to-case basis, tentative guidelines regarding the indications for structural neuroimaging in psychiatry have been suggested. These should be considered for patients who meet any of the four following criteria: -
1. Acute mental status change (including those of affect, behaviors or personality), plus any of:
- Age > 50 years
- Abnormal neurological examination.
- History of significant head trauma (i.e. Head trauma resulting in loss of consciousness or neurological sequelae)
2. New onset psychosis
3. New onset delirium or dementia of unknown etiology.
4. Prior to an initial course of ECT.
In addition to the above which focus on acute presentation; neuroimaging should also be considered when a patient’s distorted metal status proves refractory. Following these criteria a very low proportions of brain lesion associated with treatable general medical conditions could be missed. Move specifically, older age groups, psychiatric inpatients and patients with co-morbid medical illness likely will present the highest rate of positive findings. Finally an even higher percentage of patients may benefit from negative findings in a more subtle fashion i.e., as a consequence of the reassurance attained from having gross structural pathology ruled out and the primary psychiatric diagnoses solidified.
ROLE OF MRI IN CLINICAL NEUROSCIENCE: -
MRI is seen to play an important role in clinical neuroscience research in psychiatry. In general studies are done with two aims: -
- First images from large cohorts of patients and comparison subjects are reserved in order to identity pathological change that occurs in ill individuals.
- Second general research approach in to ask focused questions about the volume or shape of specific brain tissue types or structure to provide evidence regarding the involvement of these structures in the pathophysiology of specific conditions.
RECENT IMAGING MODALITIES: Recent advances in NMR and nuclear medicine techniques are finding more and more importance in pursuing active research work in Psychiatric diseases as well providing new insights into the human brain. With the advent of functional imaging, processes like memory, emotion, thought etc are being researched by scientists all over the world.
I. NUCLEAR MEDICINE (PET/SPECT):
Nuclear medicine procedures used for diagnosis and research of psychiatric conditions generally utilize PET and SPECT scans. These methods show blood flow by imaging trace amounts of radioisotopes. PET however can measure metabolism revealing how well the body is functioning. Use of radioactive tracers is well suited to studies of epilepsy, schizophrenia, Parkinson’s disease and stroke. Both PET and SPECT depict the distribution of blood into tissues, but PET does so with greater accuracy.
PET scanners watch the way the tissue cells (eg. brain cells) consume substances such as sugar (glucose). The substance is tagged with a radioisotope and brewed in a small, low energy cyclotron. The isotope has a small half-life meaning it loses half of its radioactivity only within minutes or hours of being created. Injected into the body the radioactive solution emits positrons wherever it flows. The positrons collide with electrons and the two annihilate each other releasing a burst of energy in the form of two gamma rays. These rays shoot in opposite directions and strike crystals in a ring of detectors around the patient’s head causing the crystals to light up. A computer records the location of each flash and plots the source of radiation, translating the data into an image. By tracing the radioactive substance a doctor can pinpoint areas of abnormal brain activity or determine the health of cells. Unlike PET, which specially requires a cyclotron on site, SPECT uses commercially available radioisotopes greatly reducing the cost of operation.
II. FUNCTIONAL MAGNETIC RESONANCE IMAGING (FMRI) IN PSYCHIATRY.
First, the most commonly used fMRI technique called BOLD-fMRI (Blood-Oxygen-Level-dependent fMRI) potentially offers imaging with a temporal resolution on the order of 100 milliseconds and a spatial resolution of 1-2 millimeters, which is much greater than that of PET and SPECT scanning. This means that transient cognitive events can potentially be imaged and small structures like the amygdala can be more readily resolved. Most fMRI techniques are noninvasive and do not involve the injection of radioactive materials so that a person can be imaged repeatedly. This allows imaging of a patient repeatedly through different disease states (i.e. imaging a bipolar patient through manic, depressive, and euthymic states) or developmental changes (ie. Learning cognitive stages of development, stages of grief recovery). Third, with fMRI, one can easily make statistical statements in comparing different mental states within an individual in a single session. Thus, fMRI may be of important use in understanding how a given individual’s brain functions and perhaps, in the future, making psychiatric diagnoses and treatment recommendations. It is in fact already starting to being used in presurgical planning to map vital areas like languages, motor function, and memory.
The four main applications of MRI yielding functional information in psychiatry can be categorized as: -
1. BOLD-fMRI that measures regional differences in oxygenated blood.
2. Perfusion fMRI, which measures regional cerebral blood flow.
3. Diffusion-weighted fMRI which measures random movement of water molecules and
4. MRI spectroscopy, which can measure certain cerebral metabolites noninvasively.
1. BOLD-fMRI (BLOOD-OXYGEN-LEVEL-DEPENDENT FMRI):
BOLD-fMRI is currently the most common fMRI technique. With this technique, it is assumed that an area is relatively more active when it has more oxygenated blood compared to another point in time. This is based on the principle that when a brain region is being used, arterial oxygenated blood will redistribute and increase to this area. BOLD fMRI is a relative technique in that it must compare images taken during one mental state to another to create a meaningful picture. As images are acquired very rapidly (ie. a set of 15 coronal brain slices every 3 seconds is commonly) one can acquire enough images to measure the relative differences between two states to perform a statistical analysis within a single individual. Ideally, these states would differ in only one aspect so that everything is controlled for except the behavior in question.
BOLD fMRI paradigms generally have several periods of rest alternating with several periods of activation. Images are then compared over the entire activation to the rest periods. BOLD fMRI is best used for studying processes that can be rapidly turned on and off like language, vision, movement, hearing and memory.
BOLD fMRI is very sensitive to movement so that tasks are limited to those without head movement, including speaking. BOLD fMRI is also limited in that artifacts are often present in brain regions that are close to air (ie. sinuses). Thus there are some problems in observing important emotional regions at the base of the brain like the orbitofrontal and medial temporal cortices. Another problem is that sometimes observed areas of activation may be located more in areas near large draining veins rather than directly at a capillary bed near the site of neuronal activation.
Currently, there are no indications for BOLD fMRI in clinical psychiatry, although this technique holds considerable promise for unraveling the neuroanatomic basis of psychiatric disease. It may be of potential help in sorting out diagnostic heterogeneity and treatment planning in the future. Neurologists and neurosurgeons are beginning to use this technique clinically to noninvasively map language, motor and memory function in patients undergoing neurosurgery.
2. PERFUSION fMRI:
Two fMRI methods have been developed for measuring cerebral blood flow. The first method, called intravenous bolus tracking, relies on the intravenous (iv) injection of a magnetic compound such as a gadolinium-containing contrast agent and measuring its T2 weighted signal as it perfuses through the brain over a short time period of time.
Areas perfused with the magnetic compound show less signal intensity as the compound creates a magnetic inhomogeneity that decreases the T2 signal. The magnetic compound may be injected once during the control and once during the activation task and relative differences in blood flow between the two states may be determined to develop a perfusion image. Alternatively one can measure changes in blood few over time over time after a single injection to generate a perfusion map.
This technique also only generates a map of relative cerebral blood flow, not absolute flow as in the text technique. Arterial spin labeling is a T1 weighted noninvasive technique where intrinsic hydrogen atoms in arterial water outside of the slice of interest are magnetically tagged (“flipped”) as they course through the blood and are then imaged as they enter the slice of interest.
Arterial spin labelling is noninvasive, does not involve an IV bolus injection, and can, thus, be repeatedly performed in individual subjects. Also, absolute regional blood flow can be measured which cannot be easily measured with SPECT or BOLD fMRI and requires an arterial line with PET. As absolute information is obtained, cerebral blood flow can be serially measured over separate imaging sessions such as measuring blood flow in bipolar subjects as they course through different disease states. Absolute blood flow information may be important in imaging such processes as anxiety, which may be hard to turn on and off. For instance, in social phobics, a relaxation task may be imaged on one day and anticipating making a speech may be imaged on the next day. Comparing these separate tasks in different imaging sessions would not be possible with BOLD fMRI. Arterial spin labelling has some limitations in that it takes several minutes to acquire information on a single slice of interest. Therefore, one must have a specific brain region that one is interested in examining. Also, as it currently takes several minutes to acquire a single slice, it would be tedious obtaining enough images on this slice within a single session to make a statistical statement on a given subject.
3. DIFFUSION-WEIGHTED IMAGING (DWI)
Diffusion-weighted imaging is very sensitive to the random movement of 1 H in water molecules (Brownian movement). The amount of water diffusion for a given pixel can be calculated and is called the apparent diffusion coefficient (ADC). Areas with low ADC value (ie. low diffusion) appear more intense. ADC values are direction sensitive. While it is currently unclear now diffusion-weighted imaging will be useful in studying psychiatric disorders, it hold great promise for changing the clinical management of acute ischaemic stroke by potentially refining the criteria for patients most likely to benefit from thrombolytic therapy.
4. MRI SPECTROSCOPY (MRS):
MRI spectroscopy (MRS) offers the capability of using MRI to noninvasively study tissue biochemistry. In the conventional and functional MRI techniques listed. The hydrogen atom in water is the main one that is flipped (resonated). In MRS, either 1H atoms in other molecules or other atoms such as 31P, 23Na, K, 19F or Li are flipped. Within a given brain region called a voxel, information on these molecules is usually presented as a spectrograph with precession frequency on the x-axis revealing the identity of a compound and intensity on the y-axis, which helps quantify the amount of a substance. The quantity of a substance is related is related to the area under its spectrographic peak; the larger the area, the more of a substance that is present.
The two most widely used MRS techniques involve either viewing 1H atoms in molecules other than water or 31P-containing molecules. In 1H MRS, the water signal must first be suppressed as it is much greater than the signal from other 1H-containing compounds and has overlapping spectroscopic peaks with compounds.
Compounds that can be resolved with 1H-MRS include:
a) N-acetylaspartate (NAA) which is though to be a neuronal marker that decreases in processes where neurons die;
b) Lactate which is a product of anaerobic metabolism and may indicate hypoxia;
c) Excitatory neurotransmitters glutamate and aspartate;
d) The inhibitory neurotransmitter gamma-amino butyric acid (GABA);
e) Cytosolic choline which includes primarily mobile molecules involved in phospholipid membrane metabolism but also small amounts of the neurotransmitter acetylcholine and its precursor choline;
1. Myolinositol which is important in phospholipoid metabolism and intracellular second messenger systems; and
2. Creatine molecules such as creatine and phosphocreatine, which usually have relatively constant concentrations throughout the brain and are often used as relative reference molecules (ie. one may see NAA concentration reported as the ratio NAA/creatine in the literature).
Phosphorus (31P) MRS allows the quantification of ATP metabolism, intracellular pH, and phospholipid metabolism. Mobile phospholipid, including phosphomonoesters (PME - putative cell membrane building blocks) and phosphodiesters (PDE – putative cell membrane breakdown products) can also be measured, supplying information on phospholipid membrane metabolism.
MRS can be used to identify regional biochemical abnormalities. For example, P-MRS studies of euthymic bipolar patients have revealed decreased frontal lobe PMEs (cell membrane building blocks) compared with healthy controls. However, when bipolar patients become either manic or depressed, their PMEs increase.
These findings appear to be unrelated to medication treatment. The finding of decreased frontal PMEs in euthymic bipolars has also been demonstrated in schizophrenia and speculatively accounts for the finding of decreased frontal lobe metabolism in both of these disorders. The schizophrenia finding also appears to be medication-independent.
MRS may also be of future help in the differential diagnosis of certain psychiatric diseases such as dementia. In normal aging, there is a decrease in PMEs and increase in PDEs. In early Alzheimer’s Dementia compared with healthy controls. Some believe that a decrease in NAA coupled with an increased myoinositol lever helps in differentiating probable Alzheimer’s Dementia from healthy age-matched controls as well as other dementias (usually decreased NAA but normal myoinositol levels).
With MRS, changes in metabolic activity can be measured over time within an individual scanning session. MRS can also be used to measure changes in metabolic activity between sessions, such as before and after medication treatment. For example, Satlin et al. (1997) used 1H MRS to measure midparietal lobe cytosolic choline levels in 12 Alzheimer’s subjects before and after treatment with Xanomeline, an M1 selective cholinergic agonist, or placebo. Additionally, MRS can be used to measure drug levels of certain psychotropic drugs. The magnetic elements Li and F do not naturally occur in the human body but they are fund in psychotropic drugs; lithum for Li and fluoxetine and stelazine for F. For example, studies have consistently found that the brain concentrations of lithium are about 0.5 that of serum Li levels and correlate with treatment response.
For psychiatry, MRS is a research to be used in the characterization of tumor, stroke and epileptogenic tissue and in presurgical planning.
LIMITATIONS:
MRS is restricted to studying mobile magnetic compounds. As neurochemical receptors are noted usually mobile, they cannot be measured with MRS. Thus, receptor-ligand studies are still the domain of SPECT and PET. Another problem with MRS is that due to the low concentrations of many of the imaged substances, larger areas than with water are needed to obtain detectable signals. Larger volume units imaged over longer periods are thus used with this technique, limiting both temporal and spatial resolution compared with conventional MRI and BOLD-fMRI. However, stronger magnetic fields which can spread out precession frequencies over a wider range may improve this resolution.
A brief view of recent findings are outlined.
PSYCHOTIC DISORDERS:
Research studies have identified a large number of pathologies in at last some subjects of schizophrenia for eg, the main regions sharing consistent abnormalities in schizophrenia have been frontal & temporal lobe structures. Volume decreases have been found in 62% of 37 studies of the whole temporal lobe, in 81% of 16 studies of the superior temporal gyrus and in 77% of 30 studies of the medial temporal lobe. Temporal lobe volume reduction may be uni or bilateral with deficits observed more commonly in left temporal lobe. Frontal lobe volume reductions have been reported in 55% of all published studies. Regional volume reductions have been reported in thalamus and corpus callosum. Interestingly, basal ganglia volumes may increase during treatment with typical, but not atypical neuroleptic agents. Recently studies in children have also shown findings consistent with the adult findings.
MOOD DISORDERS:
Major Depression
The spectrum of affective illness is very broad, ranging from single episodes of depressed mood, which are self-limited to life-long, treatment-refractory despondency with recurrent suicidality. Proposed that both primary and secondary mood disorders may involve abnormalities in specific frontosubcortical circuits that regulate mood. Depression is observed frequently in persons with degenerative diseases of the basal ganglia, such as Huntington’s disease, Parkinson’s disease, Wilson’s disease.
In older adults, frontal lobe atrophy and an increasing burden of T2 weighted, high signal intensity lesions have been correlated with late-life depression. Evidence suggests that depression may be seen following focal damage to critical brain regions as well as in response to diffuse brain injury. As the amygdala plays a key role in the brain’s integration of emotional meaning with perception and experience, volumetric studies of this brain structure currently are being reported. Sheline et al. have observed decreased amygdalar core nuclei volumes in depressed subjects increased amygdalar volumes in depressed patients. Mervaala et al. have noted significant amygdalar asymmetry (right smaller than left) in severely depressed subjects.
Strokes and tumors located in left sided frontal regions have been associated with new onset depression and less commonly; right-sided lesions may lead to manic symptoms. Subcortical lesions, especially of the caudate and thalamus, also can lead to mood dysregulation, with right sided lesions again being more commonly associated with mania. 30 MR studies with most consistent finding observed in 10 of 12 studies is a three-fold increase in the presence of WMH. The etiology of these WMH in bipolar patients is not clear, rates of alcohol and substance abuse, smoking cardiovascular risk factors contribute. As in schizophrenia some patients with bipolar disorder have increased lateral and third ventricular volume. Brain regions with volume deficits in bipolar include the cerebellum, especially in patients who are older or how have had multiple episodes of mania toxic effects of alcohol abuse lithium treatment.
Reduced volume and altered activity of subgenual prefrontal cortex in familial bipolar disorder has been reported. Subgenual cingulate cortex volume more recently increased amygdalar volumes have been seen in persons with bipolar disorder. Limited available data suggest that panic attacks may arise, in a minority of cases, as a consequence of ictal activity and that brain MR may identify a reasonably high yield of septo-hippocampal abnormalities in the subpopulation of panic patients who also have electroencephalogram abnormalities. Emission tomography studies generally have observed increased orbitofrontal and cingulate blood flow and glucose utilization, with decreased caudate perfusion. Hippocampal volume reductions on the order of 5% to 12% have been reported, which are of a lesser magnitude than those observed in AD or temporal-lobe epilepsy.
Neuroimaging studies of Dementing illness constitute a very active area of ongoing research. A great deal of attention has been paid to the hippocampus, as progressive atrophy has been reported to correlate with memory loss in a number of studies of both healthy adults and individuals with dementing illnesses. Recently have suggested that other regions of interest (e.g. entorhinal cortex, anterior cingulate and the banks of the superior temporal sulcus) may show larger rates of change in structural volume, over the for the hippocampal formation. Assessment of the medial occipitemporal, inferior and middle temporal gyri in demented elderly also has been suggested as a means to predict progression to AD. Alternatively, measurement of global cerebral volume also has been proposed as a means to assess disease progression. In healthy older adults, ventricular volume has been shown to increase by approximately 1.5 cm / year, suggesting that brain tissue loss is relatively slow in the absence of degenerative disorders. Frontotemporal dementia (FTD) may be distinguished from AD on the basis of anterior hippocampal atrophy (AD).
Decreases in the area of the body and posterior subregions of the corpus callosum have been reported in autistic individuals. Anorexia nervosa has been strongly associated with cerebral ventricular enlargement as well as gray and white matter deficits. Refeeding is associated with some improvement in ventricular and white matter volumes but gray matter volume deficits tend to persist, as do some neurocognitive impairments. Anorexia and bulimia may be associated with hyponatremia, which can lead to the development of central pontine myelinolysis.
Substance Use Disorders.
Alcohol-induced ventricular and sulcal enlargement have been observed by many. Regional atrophy of the corpus callosum and the hippocampus also have been reported. The cerebellum appears to be particularly sensitive to alcohol-induced damage. In addition to atrophic changes, diffuse white matter hyperintensities, suggestive of demyelination have been observed in T2 weighted examination of asymptomatic alcoholics. Signal intensity changes within the globus pallidus also have been observed in persons with cirrhosis, which may improve following liver transplantation.
Wernicke korsakoff syndrome results from nutritional deficiencies and may be precipitated by glucose administration to thiamine deficient alcoholics. The neuroanatomic change most closely associated with Wernicke Korsakoff syndrome in mamillary body atrophy although regional changes in the thalamus, orbitofrontal cortex and mesial temporal lobe also have been reported. Central pontine myelinolysis often is detected in alcoholics and presumably arises from rapid correction of electrolyte imbalance in severe hyponatremia. Extrapontine lesions also may be observed in CPM patient, affecting the cerebellar peduncles, basal ganglia and the thalamus. Marchiafava Bignami disease is a rare hemispheric disconnection syndrome typically associated with chronic alcoholism. MBD often is associated with hypointense T1 weighted or hyperintense T2 weighted lesions of the corpus callosum, suggestive of demyelination. Alcohol discontinuation and nutritional supplementation may contribute to recovery from MBD.
Stimulant Dependence.
Cocaine dependence recently has been associated with an increased incidence of WMH on T2 weighted imaging studies an incidence rate for asymptomatic stroke of approximately 3% in abstinent former cocaine users. Abuse of amphetamine and methampetamine also have been associated with cerebral ischaemia.
Other Drugs
Lipophilic adulterants present in preparations of vaporized heroin may produce signs of a toxic leukoencephalopathy. Chronic use of combined heroin and cocaine has been associated with increased pituitary volume as well as reduced prefrontal and temporal cortex volume. Solvent abuse has been linked to loss of gray white matter tissue differentiation, increased perivascular white-matter signal hyperintensities and cerebral atrophy.
CONCLUSIONS:
While there are currently no clinical indications for ordering any of these fMRI techniques, they hold considerable promise for unraveling the neurocircuitry and metabolic pathways of psychiatric disorders in the immediate future and in further helping in psychiatric diagnosis and treatment planning.
REFERENCES:
1. Magnetic resonance imaging of Brain and spine, Third Edition, Volume – I, 2002, chapter 22, Page no = 1189-1205
2. Posse S, Muller-Gartner HW, Dager SR. Functional Magnetic Resonance Studies of Brain Activation. Seminars in Clinical neuropsychiatry 1996; 1:76-88.
3. Bonder JR, Swanson SJ, Hammeke TA Morris GL, Myeller WM, Fischer M, et al. Determination of language dominance using functional MRI: A comparison with the Wada test. Neurol 1996; 46:978-984.
4. Moseley ME, Decrespigny A, Spielman DM. Magnetic Resonance Imaging of Human Brain Function. Surgical neurology 1996; 45:385-391.
5. David A, Blamire A, Breiter H. Functional Magnetic Resonance Imaging: A new technique with implications for psychology and psychiatry. Brit J Psychiatry 1994: 164:2-7.
6. Menon RS, Ogawa S, Hu X, Strupp JP, Anderson P, Ugurbil K. BOLD based functional MRI at 4 Tesla includes a capillary bed contribution: echo-planar imaging correlates with previous optical imaging using intrinsic signals. Magn Res Med 1995; 33: 453-459
7. Belliveau JW, Kennedy DN, McKinstry RC, Buchbinder BR, weisskoff RM, Cohen MS, et al. Functional mapping of the visual cortex by MRI. Science 1991; 254: 716-719.
8. Harris GJ Lewis RF, Satlin A, English CD, Scott TM et al. Dynamic susceptibility contrast MRI of regional cerebral blood volume in Alzheimer’s disease. Am J psychiatry 1996; 153: 721-724
9. Fisher M, Prichard JW, Warach S. New magnetic resonance technique for acute ischaemic stroke, JAMA 1995; 274:908-911
10. Zivan JA. Diffusion-weighted MRI for diagnosis and treatment of ischaemic stroke. Ann neurol 1997;567-568
11. Moore CM, Renshaw PF. Magnetic Resonance Spectroscopy Studies of Affective Disorders. In: Krishnan KRR, Doraiswarmy PM, editors. Brain Imaging in Clinical Psychiatry. New York : marcel-Dekker, 1997:185-213
12. Frangou S, Williams SC. Magnetic resonance spectroscopy in psychiatry: Basic principles and applications. British Medical Bulletin 1996 ; 52:474-485
13. Pettigrew JW, withers G, panchalingam K, post JF. 31P nuclear magnetic resonance (NMR) spectroscopy of brain in aging and Alzheimer’s disease. J Neural Transm Suppl 1987; 24:261-268
14. Functional magnetic resonance imaging (fMRI) for the pshychiatrist Lorberbaum JP, Bohning DE, Shastri A, Nahas Z et al.
15. Dager SR, Strauss WL, Marro KI Richards TL, Metzger GD et al. Proton Magnetic resonance spectroscopy investigation of hyperventilation in subjects with panic disorder and Comparison subjects. Am J psychiatry 1995; 152:666-672
Labels:
CT,
dementia,
MRI,
perfusion,
psychiatry
Thursday, September 25, 2008
HSV encephalitis (plain & contrast CT scans)
Wednesday, September 24, 2008
Fwd: Paper Request
---------- Forwarded message ----------
From: Atilla Çelik <dratillacelik@yahoo.com>
Date: Sun, Sep 21, 2008 at 3:43 PM
Subject: Paper Request
To: drhsdas@gmail.com
From: Atilla Çelik <dratillacelik@yahoo.com>
Date: Sun, Sep 21, 2008 at 3:43 PM
Subject: Paper Request
To: drhsdas@gmail.com
| Dear Dr. Das. I am Dr. Atilla Celik, from Istanbul, Turkey. I am working at "Haydarpasa Numune Training & Research Hospital" as a General Surgeon. I have seen your blog in recently. If it possible, I want to a copy of your published article that named "Large Adrenal Pseudocyst: Case Report with Review of Literature" in PDF format because of to cited our article "Laparoscopic management of giant adrenal cyst : Case report". Best wishes from Turkey. Dr. Atilla Celik. General Surgeon. Haydarpasa Numune Training & Research Hospital 2nd Department of General Surgery Istanbul, Turkey. +90 216 5652728 (Home) +90 532 4865625 (Cell) |
Saturday, September 20, 2008
osteoid osteoma
Osteoid osteoma is a benign lesion that accounts for approximately 10% of benign bone tumors. It occurs predominantly in children and young adults between 10 and 25, affecting males twice as often as females. The clinical presentation typically consists of pain, which is often worst at night, increased skin temperature, sweating, and tenderness in the affected region. Pain is completely relieved by salicylates in many cases.
Predilection sites are proximal femur, and diaphysis of long bones, which account for more than half of all cases, and less often foot and the posterior elements of the spine (1). Osteoid osteomas are usually detected on radiographs, typically showing a radiolucent nidus surrounded by sclerosis in the cortex of the bone. If an osteoid osteoma is suspected and radiographs are negative, skeletal scintigraphy is especially useful with a sensitivity of 100% (2). Radionuclide angiography and tissue-phase imaging often, but not always, show prominent tracer delivery and early localization. On skeletal-phase images a well-localized, focal tracer uptake is typically noted (3). Characteristic is a cloud of diffuse increase of radiotracer around the prominent focus, which is better seen on images obtained with pinhole magnification technique (4). In complicated cases computed tomography might be helpful to visualize the nidus. Scintigraphy also is contributory for treatment of patients with osteoid osteoma by ensuring complete removal of the lesion. This can be achieved either by imaging the specimen that should demonstrate a normal margin of bone around the lesion or intraoperatively with a mobile gamma camera, demonstrating that no residual activity suggestive of osteoid osteoma tissue is left (5).
Predilection sites are proximal femur, and diaphysis of long bones, which account for more than half of all cases, and less often foot and the posterior elements of the spine (1). Osteoid osteomas are usually detected on radiographs, typically showing a radiolucent nidus surrounded by sclerosis in the cortex of the bone. If an osteoid osteoma is suspected and radiographs are negative, skeletal scintigraphy is especially useful with a sensitivity of 100% (2). Radionuclide angiography and tissue-phase imaging often, but not always, show prominent tracer delivery and early localization. On skeletal-phase images a well-localized, focal tracer uptake is typically noted (3). Characteristic is a cloud of diffuse increase of radiotracer around the prominent focus, which is better seen on images obtained with pinhole magnification technique (4). In complicated cases computed tomography might be helpful to visualize the nidus. Scintigraphy also is contributory for treatment of patients with osteoid osteoma by ensuring complete removal of the lesion. This can be achieved either by imaging the specimen that should demonstrate a normal margin of bone around the lesion or intraoperatively with a mobile gamma camera, demonstrating that no residual activity suggestive of osteoid osteoma tissue is left (5).
D/D: Osteomyelitis




LARGE ADRENAL PSEUDOCYST
CASE REPORT WITH REVIEW OF LITERATURE
Authors: H.S.Das, P.Hatimota, P.Hazarika, C.D.Choudhury,
*S. K. Barua, **S.J.Baruah
Institution: Matrix, G.S.Road, Guwahati-5 and Guwahati Medical College & Hospital
Key Words: Adrenal cyst MRI
Conflict of interest: None
INTRODUCTION:
Cystic pathologies of the adrenal gland are rare with an incidence of 0.06% in 1400 autopsies. The cyst most commonly found in the adrenal gland are Endothelial cyst (45%), Pseudocyst (40%), Epithelial cyst ((9%) and Parasitic cyst (7%). Pseudocysts are consequences of haemorrhage and degeneration and are usually nonfunctional.
Pseudocysts consist of a hyalinized fibrous capsule containing nest of adrenal cortical cells and amorphous cystic contents composed of admixture of serum, blood and fibrin. Adrenal pseudo cyst vary greatly in size from microscopic to more than 50 cm with highest incidence in 5th and 6th decade with female preponderance.
Symptoms are usually associated with large cyst due to compression of surrounding viceras, pain & vague GI complaints. Imaging studies by CT scan & preferably by MRI Scan helps it to differentiate it from other adrenal pathologies. Surgical extirpation is indicated in presence of symptoms, endocrine abnormalities, complication, large size or suspicion of malignancy.
We report a case of symptomatic pseudo cyst of adrenal gland in an adult female without any hormonal abnormalities which was excised through thoraco-abdominal approach. Surgery was uneventful and patient is asymptomatic at 18 months of follow up.
CASE REPORT:
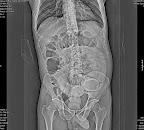
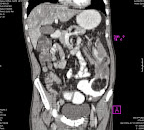
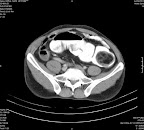
A 35 years old female presented with a one year history of non specific abdominal discomfort & occasional pain in left upper abdomen. Routine laboratory tests were within normal range. USG showed a well defined approx. 10 cm cystic mass in relation to upper pole of left kidney. MRI showed a large cystic mass separated from upper pole of the kidney with a low signal intensity in T1 weighted images and high signal intensity in T2 weighted images. A complete endocrine workup failed to detect any hormonal hypersecretion. A prospective diagnosis of left adrenal cyst was made and the lesion was excised through thoraco-abdominal approach via 11th rib.
The cyst measured approx. 10 cm in its largest dimension which on cutting open revealed chocolate colored fluid. The wall thickness varied from 0.1 to 0.2 cm. and pathological section revealed fibrous wall without any epithelial lining. The patient had an uneventful post operative recovery. She is completely symptom free at 18 months of follow up visits.
DISCUSSION:
Cysts of the adrenal gland are uncommon lesions and represent 80% of cystic adrenal masses. The etiology of pseudocyst is not well understood but is believed to arise from organization of prior haemorrhage or infectious process (1). Pseudocyst account for 40% of all cystic lesion of the adrenal gland and are consequences of haemorrhage and degeneration (2).
Most adrenal cyst are asymptomatic and less then 10 cm in diameter when discovered incidentally (3) or at autopsy (4). Symptoms appear when pseudo cyst enlarges sufficiently to cause pain and GI disturbances or become palpable (3) as in our patient. Large cyst has tendency to develop complications such as intractable haemorrhage and rupture which can manifest as a surgical emergency (5).
The haemorrhage within these lesions often give atypical imaging features on CT. Ultrasonography which could be confused with an adrenal tumor (6) . MRI is useful in differential diagnosis of adrenal cyst (7) and can differentiate it from pheochromocytoma (8).
MRI shows homogenously low intensity on T1 weighted images and high intensity on T2 weighted images in case of adrenal pseudo cyst (9, 10).
Pseudocyst may be isolated or associated with primary adrenal neoplasm such as Pheochromocytoma, adrenal adenoma, adrenocortical carcinoma and neuroblastoma (11). Pseudocyst could be confused with adrenal tumors both clinically and radiographically (12) . The more complex pseudocyst should be distinguished from cystic degeneration in adrenal malignancy and from cystic renal cell carcinoma in upper pole (2) .
Surgical excision is indicated in presence of symptoms (13), endocrine abnormality (even when subclinical), complications, large size (>5 cm) or suspicion of malignancy (14). Laparoscopic drainage (15, 16) or open surgical extirpation with preservation of adrenal tissue remains the treatment of choice. Large size, increased wall thickness or calcification are features of malignant changes which should be excised and followed up for cystic recurrence, late metastasis or adrenal endocrine dysfunction.
Other lesions that should be considered in the differential diagnosis of cystic adrenal masses are endothelial cyst, lymphangioma, epithelial cyst and parasitic (hydatid) cysts (17, 18).
REFERENCES:
1. M.A.Habra , Barry W Feig , Steven G Waguespack. , Adrenal Pseudocyst
The Journal of Clinical Endocrinology and Metabolism, 2005; 90(5) : 3067-68
2. Guensens E , De Man R, Van Oost J, Vuylsteke P., Large Adrenal Pseudocyst
, J . Belge. Radiol. 1993 ; 76(5): 322-3
3. Tagge D U , Baron P L , Giant adrenal cyst : Management and review of literature
Am. Surg. 1997; 63(8) : 744-6
4. Luciano AFavorito, Felipe M. Lott, Andre G Cavalcante. Tarumatic
rupture of adrenal pseudocyst leading to massive haemorrhage in
retroperitoneum , Int. Braz. J Urol. 2004; 30 (1), Abstract from SciELo Brazil
5. Chew S P, Sim R , Teoh TA , Low CH. , Haemorrhage in to non functional adrenal
5. Chew S P, Sim R , Teoh TA , Low CH. , Haemorrhage in to non functional adrenal
cyst- report of two cases and review of literature. Ann. Acad. Med. Singapore
1999;28: 863-6
6. Sakamoto I , Nakahara N. , Fukuda T. et. al . , Atypical appearance of Adrenal
6. Sakamoto I , Nakahara N. , Fukuda T. et. al . , Atypical appearance of Adrenal
Pseudocyst. J Urol, 1994;154(1): 150-2
7. Ito N., Fujimoto H, Arai Y, Nishimura K et. al. Two cases of adrenal cyst- the
7. Ito N., Fujimoto H, Arai Y, Nishimura K et. al. Two cases of adrenal cyst- the
meaning of imaging in diagnosing adrenal cyst. Hinyokika Kiyo, 1989;35(7): 1161-6
8. Hidetaka Suga et. al. , 14C, Jan 2003; 42(1) Crossed ref. Medline
9. Yashushi Tanuma , Makoto Kimura , Shigeru Sakai. Adrenal Cyst- A review of the
8. Hidetaka Suga et. al. , 14C, Jan 2003; 42(1) Crossed ref. Medline
9. Yashushi Tanuma , Makoto Kimura , Shigeru Sakai. Adrenal Cyst- A review of the
Japanese Literature and report of a case. International Journal of Urology, 2001;
8: 500
10. Chihangir Erem , Fatih Celik , Abdulkadir Reis et. al. Large adrenal pseudocyst
10. Chihangir Erem , Fatih Celik , Abdulkadir Reis et. al. Large adrenal pseudocyst
presenting with epigastric distress and abdominal distension ,
Medical Principle & Practice, 2005; 14: 284-87
11. Erickson L.A., Lloyd RV , Hrtman R , Thompson G. , Cystic Adrenal Neoplasm,
Cancer, 2004; 101: 1537-44
12. deBree E., Schoretsanitis G , Melissas J et. al. , Cyst of Adrenal Gland: Diagnosis and
Medical Principle & Practice, 2005; 14: 284-87
11. Erickson L.A., Lloyd RV , Hrtman R , Thompson G. , Cystic Adrenal Neoplasm,
Cancer, 2004; 101: 1537-44
12. deBree E., Schoretsanitis G , Melissas J et. al. , Cyst of Adrenal Gland: Diagnosis and
management , Int. Urol. Nephrol., 1998; 30(4): 369-76
13. N. Sezhian, D. Rimal , G Suresh . Adrenal Pseudocyst- Diagnostic Dilema
,Scottish Medical Journal, 2005; 45(2): 81
14. Manuel Suarez, Sheldon Bastacky, Vascular adrenal cyst . Final Diag. Case- 182,
13. N. Sezhian, D. Rimal , G Suresh . Adrenal Pseudocyst- Diagnostic Dilema
,Scottish Medical Journal, 2005; 45(2): 81
14. Manuel Suarez, Sheldon Bastacky, Vascular adrenal cyst . Final Diag. Case- 182,
2005, Crossed ref. Medline
15. Koksoy Ferda N , Yucel Osman , Celik Atilla et. al. Laparoscopic management of giant
15. Koksoy Ferda N , Yucel Osman , Celik Atilla et. al. Laparoscopic management of giant
adrenal cyst : Case report , Surg. Lap. End. PCN Technique, 2001;11(6); 379-81
16. Prashad R., Kumar M., Pseudocyst of adrenal gland,
Med. J, Malayasia, 2002; 57(1): 125-7
17. Satou T.,Uesugi T , Nakai Y et. al. , Case of adrenal lymphangioma with atypical
16. Prashad R., Kumar M., Pseudocyst of adrenal gland,
Med. J, Malayasia, 2002; 57(1): 125-7
17. Satou T.,Uesugi T , Nakai Y et. al. , Case of adrenal lymphangioma with atypical
lymphocytes in aspirate cytology. Diag. Cytopathol., 2003; 29: 87-90
18. Ackay MN , Akcay G, Balik AA , Boyuk A , Hydatid cyst of the adrenal gland : review
18. Ackay MN , Akcay G, Balik AA , Boyuk A , Hydatid cyst of the adrenal gland : review
of nine patients. World J Surg, 2004;28: 97-99
Figures :
1- MRI , 2- Specimen , 3- Histopathology
Figures :
1- MRI , 2- Specimen , 3- Histopathology
* Registrar Deptt of Urology, GMCH
** Prof Deptt of Urology, GMCH
Address for Correspondence:
Dr Himadri Sikhor Das,
Matrix,1st Byelane Tarun Nagar
Near Rajiv Bhawan, G.S.Road,
Guwahati-5
Tel:+0361-2595078
Email: drhsdas@gmail.com
Wednesday, July 16, 2008
GI differential Diagnoses
GI differential Diagnoses
ESOPHAGUS
Diverticular disease: pharyngocele, Zenker, Killian Jamieson, traction, pulsion, pseudodiverticula, epiphrenic
Luminal narrowing: webs, Plummer-Vinson, vascular ring, Schatzki ring, strictures (reflux, meds, skin lesions, tumor, mets, radiation, eosinophilic gastroenteritis, Crohn’s, lye, Barrett’s, infection, NGT, achalasia, scleroderma, Chagas), extrinsic compression (aorta, left bronchus, left atrium, mediastinal tumor)
High stricture: Barrett’s, radiation, caustic ingestion, CA, mets, meds, skin dz, Crohn’s
Low stricture: peptic stricture, lower esophageal ring, Barrett’s
Nodules/plaques: diffuse - reflux, Candida, glycogenic acanthosis; localized – Candida, superficial spreading CA, Barrett’s
Ulcers: distal – reflux, Crohn’s; small, mid – herpes, medications (tetracycline, doxycycline, KCl, iron, quinidine, NSAIDs, vit C, Fosamax), Crohn’s; giant – CMV, HIV
Megaesophagus: achalasia, scleroderma, distal narrowing from tumor or stricture, Chagas
Contrast extravasation: esophagitis, tumor, vomiting (MW tear, Boerhaave), TE fistula, foregut duplication cyst with communication to esophagus, iatrogenic, trauma
Solitary filling defects: intraluminal – food impaction, foreign body, fibrovascular polyp, spindle cell tumor, leiomyosarcoma, adenocarcinoma; tumor – leiomyoma, fibrovascular polyp, duplication cyst, papilloma, fibroma, hemangioma, SCC, adenocarcinoma, spindle cell tumor, lymphoma, mets (breast, lung, KS, melanoma, RCC); varices – uphill (portal HTN), downhill (SVC obstruction); extrinsic – lymph nodes, engorged vessels, aneurysms, cysts
Thickened folds: esophagitis, lymphoma, varicoid carcinoma, varices
Air-fluid level: hiatal hernia, esophageal diverticulum, CA, achalasia, scleroderma
Feline esophagus: reflux, motor disorders
Corkscrew esophagus: diffuse esophageal spasm, presbyesophagus
STOMACH
Gastritis: H pylori, erosive gastritis (corrosives, alcohol, stress, NSAIDS), granulomatous (Crohn’s, sarcoid, TB, histo, syphilis), eosinophilic, hypertrophic (Menetrier’s, ZE syndrome), recurrent gastric ulcer (ZE syndrome, PUD, drugs), radiation, emphysematous
Target lesions: gastritis (aphthoid type) – erosive (NSAID, alcohol), Crohn’s, infection (Candida, herpes, CMV); submucosal mets (large ulcer) – melanoma, KS > breast, lung, lymphoma; solitary giant bullseye (very large ulcer) – leiomyoma, sarcoma, CA, solitary met, ectopic pancreas, benign ulcer
Filling defect: bezoar, adenocarcinoma, lymphoma, leiomyosarcoma, mets, KS, endometriosis, carcinoid, leiomyoma, lipoma, polyps (hyperplastic #1), varices, ectopic pancreas, extrinsic compression from spleen/pancreas/liver
Giant rugal folds: lymphoma, Menetrier’s, ZE syndrome, gastritis, eosinophilic gastroenteritis, radiation, infection, Crohn’s, mets, varices (mimic)
Linitis plastica: scirrhous CA (#1), lymphoma, mets (esp breast), pancreatic CA (direct invasion), radiation, Crohn’s, eosinophilic gastroenteritis, corrosive ingestion, TB, sarcoid, syphilis
Antral lesions: adenocarcinoma, lymphoma, mets, Crohn’s, PUD, TB, sarcoid, HPS, pylorospasm, antral web, ectopic pancreas, erosive gastritis, caustics
Double pylorus: lesser curve antral ulcer, Crohn’s, lymphoma
Gastroenteric fistula: PUD, Crohn’s, CA, iatrogenic, surgery
Free air: surgery and laparoscopy, perforated ulcer, perforated distal bowel (IBD, diverticulitis, tumor)
UGI surgery: plication defect, marginal ulcer, bezoar, chronic gastritis, leak, obstruction, intussusception (jejunogastric), gastric CA, afferent loop syndrome, malabsorption
DUODENUM
Filling defects: benign (often 1st portion, asx) – adenoma, leiomyoma, lipoma, villous adenoma, ectopic pancreas; malignant (often distal to 1st portion, sx) – adenocarcinoma at or distal to papilla, leiomyosarcoma, lymphoma, mets (melanoma, breast, KS, carcinoid); bulb – ectopic gastric mucosa, prolapsed antral mucosa, Brunner gland hyperplasia, varices, duodenitis, Crohn’s, lymphoma, sprue, CF, polyposis, benign tumors; distal – benign lymphoid hyperplasia, ectopic pancreas, annular pancreas, ampulla of Vater, tumor, edema with impacted or passed gallstone, choledochocele; soft and changing – choledochocele, lipoma, duplication cyst
Target lesion: leiomyoma, leiomyosarcoma, met (melanoma, KS, breast, lung, lymphoma), ulcer, ZE syndrome
Luminal outpouchings: ulcer, diverticulum, choledochoduodenal or cholecystoduodenal fistula
Reverse figure 3 sign: pancreatitis, pancreatic CA
Notched duodenum: annular pancreas, post-bulbar ulcer, Crohn’s, post-op, pancreatitis, pancreatic CA
Postbulbar narrowing: adenocarcinoma, lymphoma, mets, postbulbar ulcer, duodenitis, Crohn’s, pancreatitis (extrinsic), pancreatic CA, annular pancreas, intramural diverticulum, duodenal duplication cyst, duodenal hematoma, aortic aneurysm, SMA syndrome (seen in scleroderma, lymphoma)
Papillary enlargement: >15mm; normal variant, choledochocele, papillary edema (pancreatitis, acute duodenal ulcer, impacted stone), ampullary CA
JEJUNUM AND ILEUM
Adynamic ileus: postoperative (#1); inflammatory (often sentinel loop) – pancreatitis, appendicitis, cholecystitis, diverticulitis, peritonitis; metabolic – low K+, Ca++, Mg++; medication – morphine
Mechanical SBO: adhesion, hernia, tumor, gallstone, inflammation with strictures
alabsorpmtion patterns: dilatation, dilution, delay; predominantly thick/irregular folds – Whipple’s, MAI, Strongyloides (proximal), amyloid, Giardia (jejunum), GVH, Cryptosporidium (jejunum), lymphoma, lymphangiectasia, mastocytosis, eosinophilic gastroenteritis; predominantly dilated loops and normal folds – sprue (#1), obstruction, ileus, scleroderma, medication
Thick folds without malabsorption pattern: criteria – folds >3mm, uniformly thickened if diffuse, nodular thickening (pinkyprinting) if focal with stack of coins appearance; submucosal edema – ischemia, infection, radiation, hypoproteinemia, GVH; submucosal tumor – lymphoma, leukemia, submucosal hemorrhage – Henoch-Schonlein purpura, hemophilia, anticoagulation
Tubular bowel: Cryptosporidium, sprue (proximal), lymphoma, GVH, radiation, ischemia, Strongyloides (proximal)
Nodules: mastocytosis, nodular lymphoid hyperplasia, lymphoma, mets, polyps, Crohn’s, eosinophilic gastroenteritis, TB, infection, amyloid, lymphangiectasia, Whipple’s, Waldenstrom’s macroglobulinemia
Diffuse tiny nodules: lymphoid hyperplasia (#1), hypogammaglobulinemia, Giardia, Whipple’s, Waldenstrom’s
Small bowel tumors: benign – adenoma (#1), leiomyoma (#2), lipoma, hemangioma, neurogenic tumors, Brunner gland hyperplasia, heterotopic pancreatic tissue; malignant – mets (melanoma, RCC, breast, KS), lymphoma, carcinoid (#1 primary tumor), leiomyosarcoma (large ulcerating), adenocarcinoma; polyposis syndromes
Small bowel stricture: Crohn’s, lymphoma, mets, infection, radiation, ischemia, adenoCA, extrinsic compression, NSAIDs; focal stricture with shouldering – adenoCA (#1), breast mets, TB
Coiled spring: intussusception, intramural hematoma
Large ulcerated mass (endoexoenteric): lymphoma, leiomyosarcoma, mets (melanoma), interloop abscess
Diverticula: small bowel, Meckel’s
Intraluminal filling defects: parasites (Ascaris, tapeworm), bezoar, foreign body, gallstone, lipoma
Enteric fistulas: Crohn’s, diverticulitis, CA, TB, radiation, surgery, iatrogenic
Serosal: carcinoid, serosal mets, diverticulitis, appendicitis, endometriosis
Mesenteric bowel ischemia: occlusive – emboli (afib, LV aneurysm), arterial thrombosis (atherosclerosis), venous thrombosis (portal HTN, pancreatitis, tumor, hypercoagulable state, drugs); nonocclusive – low flow state
Shortened transit time: anxiety, hyperthyroid, medication (reglan), partial SBO
COLON
Crohn’s: fold thickening, wall thickening, nodular pattern (cobblestone), string sign, aphthoid ulcers, filiform polyps, sinus tracts and fistulas, mesenteric fat stranding, creeping fat, lymphadenopathy, separated bowel loop (omega sign), pseudosacculations, strictures, asymmetric, skip lesions
UC: ahaustral, granular mucosa, filiform polyps, starts in rectum, continuous spread, backwash ileitis, crypt abscesses, strictures (worrisome)
Mass lesions: normal lymphofollicular pattern, pneumatosis coli, colitis cystica profunda, amyloid, endometriosis, ischemic colitis, polyps, polyposis syndromes, lipoma, leiomyoma, hemangioma, villous adenoma, adenocarcinoma, mets, lymphoma, hemorrhoids
Polypoid filling defects: polyps - hyperplastic (#1), adenomatous (#2), hamartomatous, post-inflammatory; polyposis – FAP, Peutz-Jeghers, juvenile polyposis, Turcot, Cronkhite-Canada, Cowden; lymphoma; pneumatosis
Carpet lesion: villous adenoma, adenoCA, polyposis, endometriosis, varices
Colonic urticaria: herpes, Yersinia, allergy, Crohn’s, ischemia
Aphthoid ulcers: Crohn’s, amebiasis, Behcet’s, CMV, herpes, TB, Yersinia (TI)
Deep ulcers: UC, Crohn’s, Behcet’s, infectious (amebiasis, TB, Salmonella, Shigella, histo, Candida, herpes, CMV), ischemic colitis, radiation
Bowel wall thickening (thumbprinting): hemorrhage – ischemia, Henoch-Schonlein purpura, hemophilia, anticoagulation; tumor – lymphoma, leukemia; edema – infectious (pseudomembranous colitis, CMV, E Coli, Salmonella, Shigella, amebiasis, typhlitis), IBD
Circumferential (apple core) or asymmetric narrowing: tumor – adenocarcinoma, serosal mets (stomach, ovarian, colon, pancreas); inflammation – diverticulitis, IBD, TB, amebiasis; other – endometriosis, pelvic abscess, epiploic appendagitis; multifocal – lymphoma, serosal mets, TB, amebiasis, Crohn’s, endometriosis
Long segment narrowing: scirrhous adenocarcinoma, lymphoma, UC, Crohn’s, ischemic stricture, radiation
Ahaustral colon: cathartic abuse (usu R colon), UC, Crohn’s, amebiasis, aging (usu L colon), scleroderma, radiation, prior ischemia
Pseudosacculations: Crohn’s, scleroderma, ischemia
Obstruction: CA, diverticulitis, volvulus, impaction, hernia
Megacolon: toxic megacolon – pseudomembranous colitis, UC, Crohn’s, amebiasis; acute distension – obstructive CA, ileus, volvulus; chronic – laxative abuse, Ogilvie syndrome, congenital Hirschsprung’s, Chagas, neuromuscular disorders (Parkinson, DM, scleroderma, amyloid), hypothyroid
Adult intussusception: usually ileoileal; tumors – polyps, lipoma, mets, lymphoma, carcinoid; idiopathic, Meckel’s diverticulum, feeding tube; no lead point consider sprue, scleroderma, Whipple’s
Pneumatosis coli: pneumatosis cystoides – COPD, asthma, CF, iatrogenic, CVD, steroids; pneumatosis intestinalis – infarcted bowel, NEC, toxic megacolon, typhlitis
Coned cecum: Crohn’s, lymphoma, mets, TB, amebiasis, typhlitis
Ileocecal deformities: Crohn’s, UC, amebiasis (spares TI), TB, typhlitis, lymphoma, adenocarcinoma, carcinoid, intussusception
Enlarged ileocecal valve: >3cm; lipomatous infiltration (#1), lipoma, Crohn’s, lymphoma, prolapsing ileal neoplasms
Cecal filling defect and nonfilling appendix: carcinoid, appendicitis, appendix stump, mucocele
Fat containing mass adjacent to colon: epiploic appendagitis, omental infarction
Proctitis: Condyloma acuminata, lymphogranuloma venereum, GC, UC, Crohn’s, HIV, herpes
Rectal involvement: serosal mets, TOA, radiation, appendicitis, diverticulitis, endometriosis
Presacral space widening: >2cm; rectal inflammation (colitis, radiation), infection, tumor, pelvic lipomatosis, edema hemorrhage
LIVER
Solid masses: hemangioma, FNH, adenoma, HCC, mets, regenerating nodules, focal fatty deposition, lymphoma
Cystic masses: infectious – pyogenic abscess, amebiasis, Echinococcus; benign – simple cysts, ADPKD, biliary cystadenoma, biloma, intrahepatic GB; malignant – necrotic tumors, cystic mets, cholangioCAcreased density: hemochromatosis, glycogen storage disease, Wilson’s, amiodarone, chemotherapy, thorotrast, anemia, regenerative nodules in cirrhosis (low T2)
Decreased density: fatty liver – obesity, alcohol, DM, steroids, chemotherapy; radiation-induced
Mottled density without focal mass: passive congestion, Budd-Chiari, geographic fatty infiltration, hepatoma, lymphoma
Hypervascular: hemangioma, hemangioendothelioma, cholangioCA, HCC, mets (islet cell, melanoma, carcinoid, RCC, thyroid, breast, sarcoma)
Hyperechoic: round – hemangioma, hyperechoic mets (hypervascular and calcified mets), HCC, fibrolamellar HCC, focal fat, lipoma, AML, Gaucher’s; linear – pneumobilia, PV gas, biliary ascariasis; multiple punctate foci – hepatitis, granulomatous infection, PCP, biliary hamartomas, pneumobilia, PV gas, vascular calcs
Multiple hypoechoic: tumor – mets, lymphoma, HCC; infection – pyogenic, amebic, Echinococcus, Candida, Schistosomiasis; other – regenerative nodules in cirrhosis, sarcoid, extramedullary hematopoiesis, hematomas, hemangiomas
Hepatic hemorrhage: iatrogenic, trauma, adenoma, HCC, pregnancy
Gas in liver: pneumobilia – ERCP, surgery, penetrating ulcer, gallstone ileus, CA, bowel obstruction; PV air – bowel necrosis > IBD, abscess, obstruction, ulcer, NEC, iatrogenic, liver transplant; abscess; emphysematous cholecystitis
Delayed retention of contrast: cholangioCA, hemangioma, fibrous tumor, scar (FNH, adenoma, fibrolamellar HCC, hemangioma)
BILIARY SYSTEM
Extrahepatic biliary dilatation: intrapancreatic (#1) – pancreatic CA, calculus, chronic pancreatitis; suprapancreatic – cholangioCA, metastatic lymph nodes; portal – cholangioCA, GB CA, surgical strictures, hepatoma; choledochal cyst
Types of obstruction: tumor – abrupt termination of duct, mass adjacent to duct; pancreatitis -–smooth, long tapering; lithiasis-related – calculus visible, meniscus sign, intrahepatic dilatation; cholangitis – sclerosing, AIDS, oriental; Caroli’s; biliary cystadenoma
Double duct sign: dilated BD and PD; pancreatitis, pancreatic CA, stone impacted in ampulla, cholangioCA, duodenal or ampullary CA
Filling defects in bile duct: stone, blood clot, parasite, sludge, tumor
Hemobilia: iatrogenic, tumor, trauma, infection
Strictures on ERCP: hilum – cholangioCA, porta hepatis nodes, GB CA; 1cm from ampulla – pancreatic CA, cholangioCA, mets; long segment – chronic pancreatitis, lymphoma; CHD at cystic duct region – Mirizzi’s, GB CA, cholangioCA; multiple intrahepatic – sclerosing cholangitis, HIV, ischemic, primary biliary cirrhosis, liver mets (rare); multiple intrahepatic and extrahepatic -–sclerosing cholangitis, HIV, ischemia
Irregular wall and filling defects: cholangitis – HIV, oriental, ascending
Pancreatic duct: stricture – pancreatic CA, chronic pancreatitis; cystic dilatation and side branches – chronic pancreatitis, IPMT; variants - annular pancreas, pancreas divisum
Cholecystectomy leaks: cystic duct remnant, duct of Luschka
GB wall thickening: >3mm; diffuse – nonfasting GB, acute cholecystitis, chronic cholecystitis, portal HTN, hypoalbuminemia, hepatitis, AIDS (cryptosporidium, CMV, MAI), ascites; focal – GB CA, mets (melanoma), cholesterol polyps, adenomyomatosis, tumefactive sludge, AIDS
GB wall hyperechoic foci: calculus, polyp, cholesterol, emphysematous cholecystitis, porcelain GB
Dense gallbladder: vicarious excretion of contrast, calculi, milk of calcium, oral cholecystogram, hemorrhage
Biliary enteric fistula: cholecystitis (gallstone ileus), PUD, tumor, trauma, surgery, Crohn’s
PANCREAS
Focal pancreatic signal abnormality: tumor, focal pancreatitis, adenopathy
Pancreatitis: causes - biliary stones, alcohol, drugs, hyperlipidemia, infection, trauma; complications – fluid collection, pseudocyst, abscess, necrosis, splenic artery pseudoaneurysm, splenic vein thrombosis
Cystic lesions: tumor – microcystic adenoma, mucinous cystadenoma, IPMT, solid/cystic and papillary epithelial neoplasm, cystic islet cell tumor; cyst – simple, pseudocyst, ADPKD, VHL, duct ectasia; abscess
Hyperechoic pancreas: CF, pancreatic lipomatosis
Hypervascular: islet cell tumor, hypervascular mets
Hypovascular: adenocarcinoma, focal chronic pancreatitis
SPLEEN
Anatomic variations: accessory spleen, lobulations, wandering spleen, polyspenia, asplenia, splenosis (s/p trauma)
Focal splenic lesions: tumor – mets (lymphoma, melanoma), hemangioma, lymphangioma, hamartoma; infection (often calcified) – abscess, Candida, TB, MAI, Schistosomiasis, PCP; other – infarct, septic emboli, hematoma, cyst (simple, hydatid) pancreatic pseudocyst, fatty nodules in Gaucher’s
Microabscess pattern: Candida, MAI, TB, PCP, bacterial, fungal, Gaucher’s, sarcoid, KS, lymphoma, mets
Scalloped contour: infarcts, septic emboli, hematoma, metastatic implants, pseudocyst
Splenic cyst: primary – congenital, true; secondary – calcified, false, prior infarct, trauma, infection, echinococcus, pancreatic pseudocyst
Splenic calcifications: TB, histo, PCP, phleboliths, hemangioma
Splenomegaly: tumor – lymphoma, leukemia; infection – infectious mono, histo, sarcoid; metabolic – Gaucher’s, amyloid, hemochromatosis; trauma; vascular – portal HTN, hematologic disorders
PERITONEAL CAVITY
Peritoneal mets: ovarian, stomach, colon, pancreas
Pseudomyxoma peritonei: mucinous cystadenoCA from ovary or appendix, mucocele
Peritoneal fluid collections: ascites, urinoma, biloma, seroma, lymphocele, pseudocyst, CSFoma; complex – abscess, hematoma, pseudomyxoma peritonei, pancreatic necrosis
Intraperitoneal calcifications: arterial calcs, appendicolith, mesenteric node, gallstone, pancreatic calcs, porcelain GB, renal/ureteral stone, nephrocalcinosis, old hematoma, abscess, fibroid, fetal skeletal part, phlebolith, teratoma, echinococcal cyst, mucinous tumor
MISC
General GI DDx: Crohn’s, lymphoma, TB (infection), mets, CA, radiation, ischemia
Mucosal: acute angle, absence of normal mucosal pattern, irregular fuzzy margin
Submucosal: obtuse angle, presence of normal mucosal pattern, smooth distinct margin
Extrinsic: spiculation, tethering
AIDS: infection – CMV, Candida, herpes, Cryptosporidium, MAI; tumor – KS, lymphoma; esophagus – ulcers (Candida, CMV, herpes, HIV), sinus tracts (TB, Actinomycosis); proximal small bowel – ulcers (cryptosporidium), nodules (KS, lymphoma, MAI); distal small bowel – enteritis (TB, MAI, CMV); colon – colitis (CMV, pseudomembranous), typhlitis; rectum – herpes, lymphoma; biliary – strictures (CMV, Cryptosporidium); liver and spleen – KS, lymphoma, Candida, TB, MAI, PCP
Abdominal trauma: liver laceration (#1), splenic lac, renal trauma, bowel hematoma, pancreatic fx, GB injury, adrenal hemorrhage
Abdominal complications after cardiac surgery: GI hemorrhage, cholecystitis, pancreatitis, perforated peptic ulcer, mesenteric ischemia, perforated diverticulitis
Low density lymph nodes: TB, MAI, lymphoma, testicular tumor, mucinous adenoCA, Whipple’s
Cystic abdominal mass: abscess, loculated ascites, panc pseudocyst, ovarian cyst or tumor, lymphocele, cystic lymphangioma, enteric duplication cyst, cystic teratoma
Mesenteric mass: lymphoma, mets, carcinoid, mesenteric fibromatosis, mesothelioma
Large LUQ mass: stomach (leiomyosarcoma), pancreas (pseudocyst, nonfunctioning islet cell tumor, mucinous tumor), adrenal (carcinoma), spleen (lymphoma), kidney (RCC, lymphoma)
RLQ inflammation: appendicitis, Crohn’s, cecal diverticulitis, perforated cecal CA, mesenteric adenitis, PID
Volvulus: gastric (organoaxial, mesenteroaxial), midgut, colon (sigmoid, cecal)
Hernia: paraesophageal, paraduodenal, inguinal, umbilical, Spigelian, lumbar, Richter’s, incisional
Abdominal wall: mets (melanoma, NF, iatrogenic seeding), rectus sheath hematoma (trauma, anticoagulation)
Ascites: cirrhosis, mets, CA, hypoalbuminemia, CHF, pancreatitis
Gasless abdomen: obstruction with fluid-filled bowel, severe vomiting, high obstruction, achalasia, impaired swallowing, continuous NG suction
Subscribe to:
Posts (Atom)